If not for flawed tracking, medical mistakes would be the third-leading cause of death, researchers at Johns Hopkins say.
By Marshall Allen & Olga Pierce
(Photo: Carl Court/Getty Images)
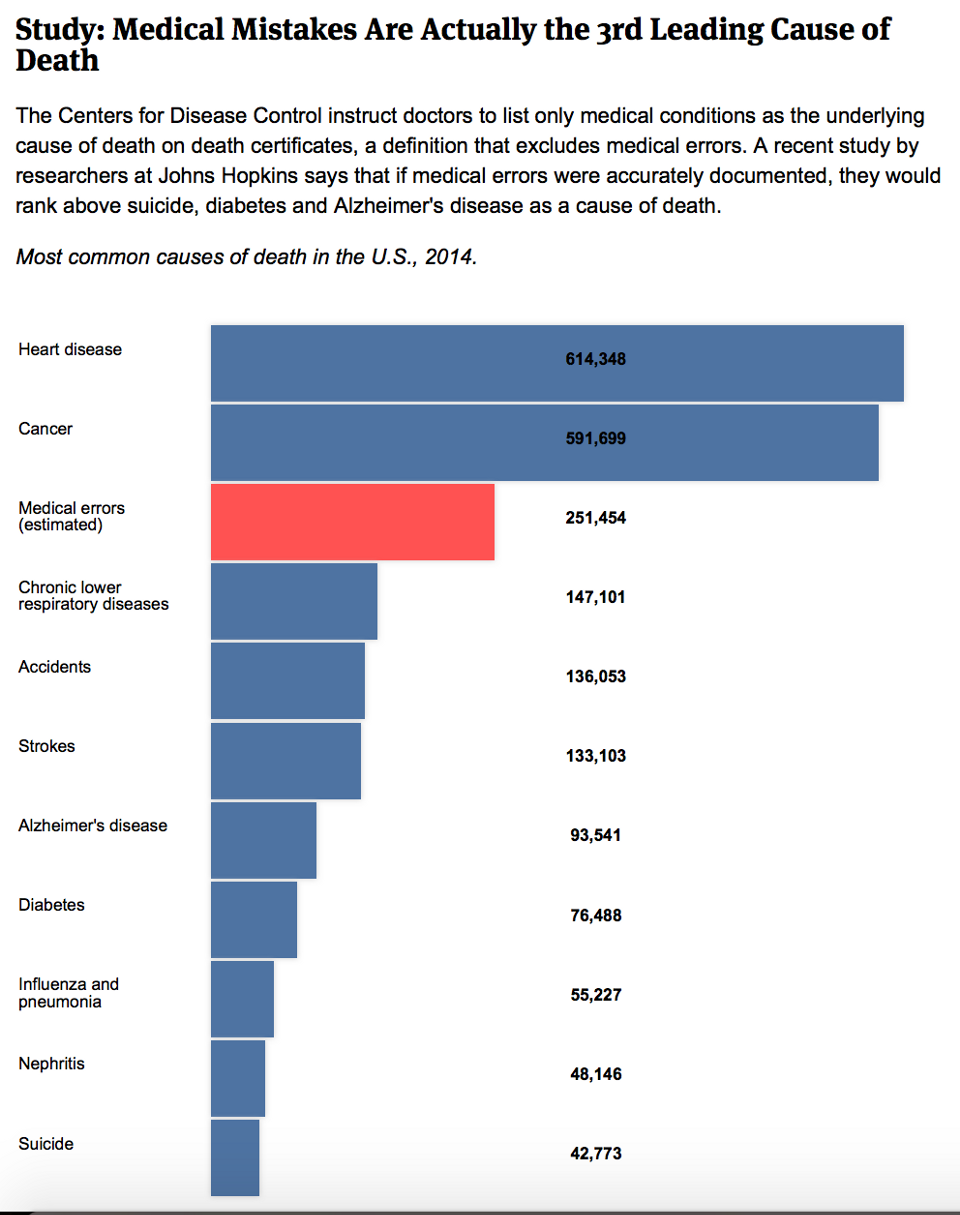
A study by researchers at Johns Hopkins Medicine says medical errors should rank as the third-leading cause of death in the United States — and highlights how shortcomings in tracking vital statistics may hinder research and keep the problem out of the public eye.
The authors, led by Johns Hopkins surgeon Dr. Marty Makary, call for changes in death certificates to better tabulate fatal lapses in care. In an open letter, they urge the Centers for Disease Control and Prevention (CDC) to immediately add medical errors to its annual list reporting the top causes of death.
Based on an analysis of prior research, the Johns Hopkins study estimates that more than 250,000 Americans die each year from medical errors. On the CDC’s official list, that would rank just behind heart disease and cancer, which each took about 600,000 lives in 2014, and in front of respiratory disease, which caused about 150,000 deaths.
The Johns Hopkins’ authors said the inability to capture the full impact of medical errors results in a lack of public attention and a failure to invest in research.
Medical mistakes that can lead to death range from surgical complications that go unrecognized to mix-ups with the doses or types of medications patients receive.
But no one knows the exact toll. In significant part, that’s because the coding system used by CDC to record death certificate data doesn’t capture things like communication breakdowns, diagnostic errors, and poor judgment that cost lives, the study says.
“You have this over-appreciation and overestimate of things like cardiovascular disease, and a vast under-recognition of the place of medical care as the cause of death,” Makary said in an interview. “That informs all our national health priorities and our research grants.”
The study was published in the BMJ, formerly the British Medical Journal.
Bob Anderson, chief of the mortality statistics branch for the CDC, disputed that the agency’s coding is the problem. He said complications from medical care are listed on death certificates, and that codes do capture them. The CDC’s published mortality statistics, however, count only the “underlying cause of death,” defined as the condition that led a person to seek treatment.
As a result, even if a doctor does list medical errors on a death certificate, they are not included in the published totals. Only the underlying condition, such as heart disease or cancer, is counted, even when it isn’t fatal.
Anderson said the CDC’s approach is consistent with international guidelines, allowing U.S. death statistics to be compared with those of other countries. As such, it would be difficult to change “unless we had a really compelling reason to do so,” Anderson said.
The Johns Hopkins’ authors said the inability to capture the full impact of medical errors results in a lack of public attention and a failure to invest in research. They called for adding a new question to death certificates specifically asking if a preventable complication of care contributed.
“While no method of investigating and documenting preventable harm is perfect,” the authors write, “some form of data collection of death due to medical error is needed to address the problem.”
Anderson, however, said it’s an “uncomfortable situation” for a doctor to report that a patient died from a medical error. Adding a check box to the death certificate won’t solve that problem, he said, and a better strategy is to educate doctors about the importance of reporting errors.
“This is a public-health issue, and they need to report it for the sake of public health,” he said.
Dr. Tejal Gandhi, president of the National Patient Safety Foundation, said her organization refers to patient harm as the third-leading cause of death. Better tracking would improve funding and public recognition of the problem, she said.
“If you ask the public about patient safety most people don’t really know about it,” she said. “If you ask them the top causes of death, most people wouldn’t say ‘preventable harm.’”
Dr. Eric Thomas, a professor of medicine at the University of Texas Medical School at Houston whose research was cited in the Institute of Medicine’s landmark “To Err is Human” report, said existing estimates aren’t precise enough to support immediately listing errors as the third-leading cause of death.
But collecting better cause-of-death data is a good idea, said Thomas, who agreed that medical errors are underreported.
“If we can clarify for the public and lawmakers how big a problem these errors are,” he said, “you would hope it would lead to more resources toward patient safety.”

||
This story originally appeared on ProPublica as “Study Urges CDC to Revise Count of Deaths From Medical Error” and is re-published here under a Creative Commons license.




