Dr. Jerome Kabakyenga has just walked a pair of visitors through a pair of vividly different Ugandan hospital laboratories — one ultramodern, the other an outdated relic. In the first, highly trained technicians investigate blood samples using a battery of high-throughput computerized systems. The brightly lit, air-conditioned facility is spotless. In the second lab on Kabakyenga’s tour, there’s little equipment beyond a clutter of microscopes, a pair of old refrigerators and a few centrifuges. The technicians here depend on daylight from a set of dusty windows, one of which is cracked. As he completes the tour, Kabakyenga, who is the dean of medicine at the Mbarara University of Science and Technology in western Uganda, does his best not to say what’s on his mind. He knows the contrast between the two facilities — both of which serve a population of about 1 million Ugandans in the region around the city of Mbarara — tells a startling story about medicine right across Africa. But today, Kabakyenga wants to let the labs do the talking.
In this tale of two labs, the state-of-the-art facility is one that provides HIV/AIDS testing; it was paid for by wealthy foreign donors. The other facility is the Mbarara regional hospital’s antiquated general diagnostic laboratory, which operates on a shoestring budget provided partly by Kabakyenga’s university department. The disparity between the two labs means that, while many HIV/AIDS patients can get reasonable care, vastly larger numbers of patients — in an area long stricken with numerous other killer diseases besides AIDS — cannot. In a hospital where up to 20 percent of patients have HIV, investment in an HIV/AIDS lab is critically important. But the lack of resources for testing and treating diseases other than HIV/AIDS is disastrous: “We can do rapid and comprehensive viral load analyses for HIV patients,” Kabakyenga says, using the careful cadences of a scholarly man who risks straying into a political minefield. “But we can’t always manage a timely malaria test.”
Few places have enjoyed peace amid continuous political bloodbaths as long as Mbarara, which is the largest city in mostly rural western Uganda. In the 1970s, when much of Uganda descended into political butchery under the notorious dictator Idi Amin, Mbarara’s small population was largely spared. In the 1980s, when civil war ravaged the country, Mbarara’s handful of paved streets again served as sanctuary. In the 1990s, when a million people died during a genocide in Rwanda, just 60 miles away, Mbarara remained placid. Today, the lucky streak continues: With millions dying in the war-torn Democratic Republic of the Congo, just 80 miles to the west, Mbarara is largely untouched. But peaceful as it is, Mbarara and the region around it have frighteningly high death rates, especially among mothers and children. Meager medical services and high levels of malaria, tuberculosis, HIV/AIDS and numerous other killers mean that young children in western Uganda are about 25 times more likely to die before the age of 5 than in the U.S.

And even while attention to AIDS grew rapidly in Uganda and across Africa in recent years, many diseases that kill far more people — especially women and children — remain neglected. “For years, maternal and child health have been side issues, while concern for HIV was at the forefront,” Kabakyenga explains. “Now, some of us think it’s time these other issues get attention as well.”
It is the rainy season in Buhihi, a village of about 100 families located about a two-hour drive north of Mbarara. This is an area of banana plantations and deep rural poverty. Alice Tumisine is a subsistence farmer who depends on 2 acres of land to raise her family. Today, two of her three children are sick. The youngest, who is 3 years old, has a cough and seems sluggish. The middle child, who is 6, has a painful skin rash around her neck. Both children sit on a straw mat that divides the dirt floor in their home, a two-room mud-and-wattle house surrounded by banana trees.
A thin sheet of tattered cloth is all that shields Tumisine’s doorway from the rain, and although the weather is mild, the children seem cold in a home without heat. “I’m not sure why they are ill,” she says. “They have both been to the local government-run health clinic to receive medication for malaria and diarrhea many times.”
A neighbor, Richard Nuwagira, is trying to help. As part of a program organized by Kabakyenga at Mbarara University of Science and Technology, Nuwagira has been instructed in a set of basic concepts in managing child illnesses, including malaria, tuberculosis, diarrhea, pneumonia and HIV/AIDS. He has helped Tumisine take the children to the local government clinic in the past, and he’s now pushing her to go back to the clinic tomorrow. “I also worry about Alice,” he says discreetly. “I think she needs some tests as well.”
Nuwagira’s decision to volunteer as a village health coordinator stemmed in part from the little perks — a new pair of boots, an occasional tank of gas for his tiny motorcycle — that came with the role, he acknowledges. But mostly, he says, he volunteered because, at 47, he’s now one of the oldest remaining men in the community. Over his life span, he’s seen a tsunami of death and disease. Malaria, pneumonia, tuberculosis and all manner of tropical diseases and parasites have always plagued Buhihi, he explains. But in the mid-1980s, he recalls, AIDS struck the village as well. “Many people died here from AIDS,” he murmurs while staring down at the puddles growing around his boots in the rain. “Too, too many.”
The arc of Uganda’s AIDS epidemic almost exactly matches the time span of Nuwagira’s adult life. Uganda was an early hot spot in Africa’s horrific AIDS disaster, and by the late 1980s, the country was a byword for the disease’s ravaging progress across the rest of the continent. That notoriety spurred action: In the early 1990s, the Ugandan government adopted a mix of successful AIDS prevention strategies based on massive public information campaigns emphasizing safe sex. By the end of the decade, the epidemic’s spread had been largely staunched — making Uganda something of a poster child among international AIDS campaigners. Partly as a result, in recent years, Ugandan AIDS programs have benefited from international assistance on a huge scale. And thanks to that, health workers and activists living in even remote quarters of the country, such as Nuwagira, have now begun to think that other health problems — especially the handful of easily preventable diseases responsible for killing roughly four times as many Ugandans as AIDS — also require urgent attention from wealthy international donors.
Much of the money flowing into Ugandan AIDS programs comes from Washington. In 2003, then-President George W. Bush won distinction as the biggest spender in the history of international AIDS efforts by launching The U.S. President’s Emergency Plan for AIDS Relief. Through PEPFAR, in just five years, U.S. appropriations for international HIV/AIDS prevention and treatment more than tripled, from about $5 billion to more than $18 billion. But some countries have been luckier than others: For the war-ravaged Democratic Republic of the Congo, with a population of 68 million and an HIV prevalence of 3.2 percent, about $47 million was earmarked between 2003 and 2008. For neighboring Uganda, with a smaller population of 27 million but a higher HIV prevalence of 5.4 percent, $880 million was made available.
PEPFAR’s worldwide achievements have been substantial. In the five years after President Bush launched the program, it extended care to more than 10 million people affected by HIV/AIDS. About 57 million people received HIV counseling and testing, and 2.2 billion condoms were distributed. Support was given for the prevention of mother-to-child transmission of HIV during nearly 16 million pregnancies, and antiretroviral prophylaxis was supported for nearly 1.2 million pregnant women found to be HIV-positive, allowing nearly 240,000 infants to be born HIV-free. Some 2.1 million HIV-infected patients received antiviral drug treatment, saving an estimated 3.28 million adult years of life through the end of September 2009.
Such success stories are extremely rare in the history of disease-control in poor regions like sub-Saharan Africa. But in a report released last November praising PEPFAR and another massive effort, The Global Fund to Fight AIDS, Tuberculosis and Malaria, a team of researchers from Médecins Sans Frontières, a medical aid group that offers health care in war zones but has also provided AIDS care to 140,000 patients in 30 countries, described the global response to AIDS in recent years as exactly that — an overall success. “As a result of widespread public pressure and an eventual worldwide mobilization of resources,” MSF noted, “HIV/AIDS care, treatment and prevention programmes have expanded massively. There are now four million people alive as a result.”
But far from suggesting that anything like a celebration was in order, MSF offered a stark warning: “Rather than looking for ways to leverage and replicate the success of the AIDS public health revolution to improve global health, there are increasing calls for a diversion of foreign aid away from HIV/AIDS and towards other health priorities. While there is clearly a need to give urgent and additional resources to an array of global health priorities, not least maternal and child health, cutting HIV/AIDS funding is not the answer.”
In the war on preventable international diseases, relatively well-financed AIDS fighters have begun to attract resentment from fighters of less bankable diseases. With 3 million new people infected with HIV every year, huge resources are required to combat the epidemic, those involved primarily with fighting other diseases agree. But many experts, including Kabakyenga, say the time has come to find matching resources for the 530,000 women who die annually from largely preventable complications related to pregnancy and the 8.8 million children who die every year, many from easily treatable or vaccine-preventable conditions and malnutrition.
Propelled by this logic, efforts to rebalance international health care assistance to include formerly neglected killers alongside HIV/AIDS are gathering momentum. The Obama administration, for example, has decided not to increase funding for PEPFAR as it promotes a new six-year, $63 billion Global Health Initiative focusing on overall family health rather than any one specific disease. Similarly, the British government, which led the charge for support for HIV/AIDS among the G8 league of rich nations in 2003, has now “downscaled resources for HIV/AIDS, shifting support to maternal and child health,” MSF notes.
But by focusing aid on “strengthening health systems,” MSF complains in its call for a continued focus on AIDS, Britain has adopted “a broad and largely unmeasurable goal.” Is this turn toward diversifying disease-fighting programs alongside AIDS efforts — rather than continuing to boost AIDS budgets — a perverse effort aimed at punishing the success of AIDS fighters? Maybe so, MSF says. The group’s choice of a title for its report punched home exactly that point: “Punishing Success? Early Signs of a Retreat from Commitment to HIV/AIDS Care and Treatment.”
Well before MSF challenged the prospect of a diversion of foreign aid away from HIV/AIDS toward other health priorities, resentment within the international health community about the focus on AIDS had begun to percolate. Some voices critical of what has been labeled “AIDS exceptionalism” have been very blunt. The U.S. faith-based group Bread for the World, for example, has been particularly upfront. In a recent report, the group pointedly noted that in the case of Ethiopia, in 2008, “approximately 80 percent of U.S. poverty-focused development assistance — roughly $400 million — went to fight HIV/AIDS.” In a country where famine and malnutrition kills far more people than AIDS, the group would like to see more resources given to agricultural assistance alongside AIDS programs.
In the struggle to control HIV/AIDS, nutrition is critically important, Bread for Life notes. To drive that point home in a report several years ago, the group quoted Peter Piot, a former executive director of UNAIDS, recounting his experience in talking with HIV-positive women in Malawi: “As I always do when I meet people with HIV/AIDS and other community groups, I asked them what their highest priority was. Their answer was clear and unanimous: food. Not care, not drugs for treatment, not relief from stigmas, but food.”
Bread for Life’s perspective is not an isolated one. A spike in global food prices in recent years has pushed at least 100 million more people into hunger, according to a World Health Organization estimate, which means that at least 1 billion people now go hungry. Even where starvation does not pose a direct threat to life, malnutrition poses huge health risks, especially to children and mothers suffering from disease.
Jude Kimbowa, a pediatrician at the Mbarara Regional Referral Hospital who works with Kabakyenga, notes that malnutrition is almost always a complicating factor in diseases he treats — whether it is HIV, malaria, TB or any of a dozen or more major killers. But funding for research into how to tackle anything but HIV/AIDS is almost nonexistent, he laments.
During a recent shift on the malnutrition ward where Kimbowa works, 13 babies were being nursed back to life in a room almost devoid of basic medical equipment. Much of the care was being administered by family members, many of whom were living outdoors on the hospital grounds. The hospital itself operates on a shoestring budget, Kimbowa noted. And that means there are few resources to investigate ways to help improve children’s health — unless HIV/AIDS is involved. “I wouldn’t say we’re at the point of hopelessness,” Kimbowa said, “but there is a lot out there that we have not been able to look at. Take malnutrition. We did a small retrospective in 2008 and found that 80 percent of admissions had some degree of malnutrition, and 40 percent were severe. Almost no one is looking at other common childhood illnesses — diarrhea, pneumonia, intestinal infestations.”
In a review of the global malnutrition crisis published in 2008, the U.K. medical journal The Lancet estimated that about 3.5 million mothers and children die annually due to nutrition-related factors. Suboptimum breast-feeding alone was estimated to cause 1.4 million child deaths. So how expensive would it be to tackle this problem? According to an analysis prepared for the World Bank by Sue Horton, a Canadian economist who specializes in costing child and maternal survival strategies, about $10 billion. Currently, international donors stump up about one-tenth of that amount.
Malnutrition crusaders are not the only ones clamoring for resources to match the HIV/AIDS war chest. A recent report on immunization published by the U.N. children’s fund and the World Health Organization poses — and then swiftly answers — a blockbuster question: “If children’s lives are worth saving — and who would doubt that they are; if vaccines save lives — and the evidence is clear that they do; and if the world has the means of making, buying, and using vaccines, as it surely does: then why are children still dying from diseases that vaccines can prevent? The answer to this conundrum lies perhaps in the difficulty of choosing between conflicting priorities.”
The numbers compelling action on immunization are galvanizing: Along with clean water and better sanitation, immunization is credited with reducing the number of children under 5 dying every year from 17 million in 1970 to 10.5 million in 2000 and 9.2 million in 2007. “With the exception of safe water, no other modality, not even antibiotics, has had such a major effect on mortality reduction,” note the editors of Vaccines, a medical school textbook.
Progress on immunization in 72 of the poorest countries has been substantial in recent years, and for that, according to UNICEF and the World Bank, credit goes to the GAVI Alliance, (formerly known as the “Global Alliance for Vaccines and Immunisation”) a vaccine-financing partnership whose members include UNICEF, WHO, the World Bank and The Bill & Melinda Gates Foundation, as well as donor and developing country governments, private companies and innumerable community groups.
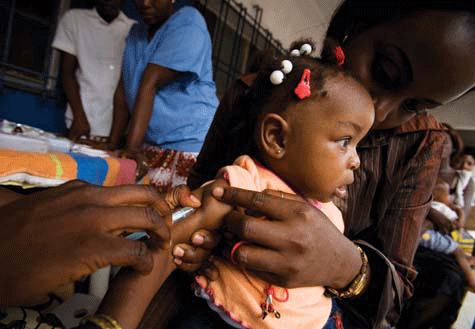
(Courtesy of GAVI)
GAVI has vaccinated 200 million children and averted an estimated 3.4 million premature deaths since 2000, all at a cost since 2000 of $2.7 billion, even as funding commitments for immunization programs shrank. By any measure, at about $18 per child, immunization is a startlingly cost-effective health intervention. Even so, it’s estimated that 24 million children — almost 20 percent of the children born each year — still do not get the routine immunizations required in the first year of life. Ensuring they did so, however, would be far cheaper than almost any other approach to mass public health assistance in developing countries: For a mere $1 billion per year on top of current immunization expenditures, new and existing vaccines could be delivered to all children in the 72 poorest countries, GAVI says.
According to the WHO, if all the vaccines now available against childhood diseases were widely adopted, and if countries could raise vaccine coverage to a global average of 90 percent, by 2015 an additional 2 million deaths a year could be prevented among children under 5 years old — all at a fraction of the cost of existing HIV/AIDS programs with similar targets.
Achieving comprehensive global child immunization is among the greatest, entirely doable and comparatively affordable humanitarian opportunities in history — one that would dwarf the benefits of the eradication of smallpox, which cost $100 million over a 10-year period up to 1977 and has been saving vast numbers of lives, and an estimated $1.3 billion a year in treatment and prevention costs, ever since.
The calls for a rebalancing of the focus on HIV/AIDS to include equal attention to malnutrition, vaccination and neglected diseases grew from a significant body of peer-reviewed research strongly inflected with an explicitly moral complexion.
One of the earliest and toughest such assessments was published in 2006 in PLoS Medicine — a medical journal dedicated to open access without commercial constraint — under the seemingly obscure title “Incorporating a Rapid-Impact Package for Neglected Tropical Diseases with Programs for HIV/AIDS, Tuberculosis, and Malaria.”
The paper’s authors were a team composed of the distinguished British and American parasitologists Peter Hotez, David Molyneux, Alan Fenwick and Eric Ottesen, writing alongside the famous American development economist Jeffrey Sachs and his wife, Sonia Ehrlich Sachs, an international public health project coordinator. Hotez and his team were intent on using the journal as a scientific platform to bluntly call for a reconsideration of the focus on HIV/AIDS in moral terms cast around the need for a “comprehensive pro-poor health policy.”
To do so, Hotez and his co-writers took the unusual step in a scientific journal of tacking a quote from Elie Wiesel — the Nobel Prize-winning Holocaust writer — above their scientific review. The words that they borrowed from Wiesel are stark: “The age of hypocrisy has been succeeded by that of indifference, which is worse, for indifference corrupts and appeases: It kills the spirit before it kills the body. It has been stated before, it bears repeating: The opposite of love is not hate, but indifference.”
Neglected Tropical Diseases
Almost everyone in the world’s “bottom billion” has at least one of a dozen or so diseases that mostly ignored by Western medicine and pharmaceutical companies. For descriptions and symptoms those named among Hotez’s neglected tropical diseases, read:
“List of Neglected Tropical Diseases.”
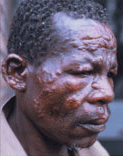
Having directed readers to see their paper not only as a piece of detached scientific analysis but as a call to moral action, Hotez and his team phrased a tough argument, calling attention to a wide array of “neglected” tropical diseases and infections — the list included leishmaniasis, human African trypanosomiasis, Chagas disease, trachoma, leprosy, Buruli ulcer, hookworm, ascariasis, trichuriasis, lymphatic filariasis, onchocerciasis, guinea worm, schistosomiasis, Cysticercosis, and food-borne trematodiases.
According to Hotez’s group, evidence was growing that this set of neglected tropical diseases may not only “threaten the health of the poor as much as HIV/ AIDS, tuberculosis, or malaria, but even more importantly, may have effective treatment and prevention strategies that can be delivered for less than US $1 per capita per year.”
Noting that increased efforts by G8 nations and U.N. agencies to improve the health of the world’s poorest 3 billion people has focused on fighting HIV/AIDS, tuberculosis and malaria, Hotez and his team complained that “conspicuously absent from these activities, however, has been commensurate advocacy for a group of diseases that exclusively affect the poor and the powerless in rural and impoverished urban areas of developing countries.”
The time had come, they argued, for a rethink: “Given the compelling logic and the very modest costs of embracing neglected tropical disease control efforts, it is surprising that those aiming to control the big three have largely ignored these opportunities,” they charged. “For too long the big three partnerships have worked in isolation.”
If any single individual deserves greatest credit for mobilizing rich nations, international agencies, corporations and individuals to devote money to AIDS in recent years, he may well be Stephen Lewis, a former Canadian diplomat who served as the U.N. Secretary General’s Special Envoy for HIV/AIDS in Africa from June 2001 until the end of 2006. It was during this period that the G8, the U.S. and many other wealthy governments, as well as corporate leaders and mega-philanthropists like Bill Gates, were finally persuaded — largely by Lewis and other high-flying advocates, including former President Bill Clinton — to begin devoting serious money to fight the AIDS pandemic in the world’s poorest, sickest places, especially sub-Saharan Africa.
These days, Lewis acts as a fundraiser for international AIDS programs, and he serves as the only non-American on the board of the Clinton Health Access Initiative, which aims to build on the Clinton’s success in persuading pharmaceutical companies to dramatically lower drug costs in 70 countries. As deputy director of UNICEF for five years in the late 1990s before taking on the job as the world’s senior AIDS diplomat, Lewis notes, “I spent as much time on oral rehydration and on malnutrition and on diarrhea and on acute respiratory infections and on pneumonia as on the emerging AIDS dilemma.”
Having seen all sides of the disease disaster, Lewis passionately decries any suggestion that money might now be diverted away from AIDS toward fighting other diseases.
Whether more lives could be saved by tackling different diseases that are cheaper to treat is a question he rejects. “It is a false and destructive dichotomy to pit one set of diseases against another,” he insists. “Everybody talks about the AIDS exceptionalism. Nobody talks about the moral obligation of the Western world to provide the money to do both.”
That money, Lewis notes, was promised long ago, in 1969, when the world’s wealthy nations agreed that seven-tenths of 1 percent of their gross national products should be devoted to helping poor countries. “We’re less than halfway there. And now, with the so-called international financial crisis, we’re declining further,” he says. “And the money that should be available for this — which is a larger pie, not a diminution of money for AIDS — is what everybody should be fighting for. Instead, the AIDS activists have been rendered on the defensive.”
While making this protest, Lewis adds that the money amassed for international AIDS control has cleared a path for new programs now required to fight other diseases as well. AIDS treatment and prevention efforts, Lewis believes, have become a kind of vector for the control of other diseases in numerous countries formerly bereft of such capacity: “Much of the health systems’ strengthening in these countries — much of the human resources necessary to respond to the entire basket of issues — is happening because of AIDS,” Lewis says. “It’s hard to get one’s mind around the positive things that have flowed from so ghastly an experience. But it is true that the development of laboratories across the continent, the development of research across the continent, the extraordinary sophistication for vaccine development has spawned a degree of public health awareness and activity that is really quite marvelous.”
Having come this far, Lewis argues, the “sheer criminal delinquency” of rich nations that fail to provide sufficient funding for comprehensive disease control cannot be ignored or used to justify scaling back the attack on AIDS: “All of them have to be funded and not one at the expense of the other. You don’t sacrifice AIDS because the Western world has defaulted on its obligations and on its promises.”
For Jerome Kabakyenga, what started as a nagging issue has now become a burning concern.
After 20 years of watching while international support for HIV/AIDS programs multiplied, the imperative to start tackling the health of children and mothers alongside HIV/AIDS has become unavoidable. Driven by frustration with the endless preventable carnage, late last year, Kabakyenga decided to step down as dean of Medicine at the Mbarara University of Science and Technology and get back to Bushenyi, a rural district with tremendously high death rates among mothers and children. It was in Bushenyi that he first started practicing medicine — much of it focused on women and children — 20 years ago as a young doctor.
In the years ahead, Kabakyenga plans to save as many lives as possible. “For the next phase of my career, I want to focus on studying obstructed prolonged labor,” Kabakyenga explained in a meeting at his spacious medical school office a few weeks after he made the decision to quit. “We are losing a lot of kids’ mothers in childbirth. I want to do something about it.”
To kick-start this new work, Kabakyenga will draw from a substantial cash award he received last year from the Global Health Research Initiative, a Canadian agency that has pushed in recent years to diversify international heath research to include other killers alongside HIV/AIDS.
In stepping back from the prestige of his position as dean, Kabakyenga acknowledges that he’s surrendering the power to direct other researchers toward new priorities. But with funding still almost nonexistent for anything but HIV/AIDS research in Africa, Kabakyenga says he won’t wait.
“The challenge is to get the prominence of child health and maternal health to reach the level that HIV has achieved,” he says. But rather than waiting for the international donors to figure this out, Kabakyenga has decided to plunge in. “For me, it’s a personal decision,” he explains. “The death rate for mothers and children is simply overwhelming. I’ve been taken up by the passion of this issue.”
Sign up for the free Miller-McCune.com e-newsletter.
“Like” Miller-McCune on Facebook.
Follow Miller-McCune on Twitter.
Add Miller-McCune.com news to your site.





